Why Do Hereditary Pathogenic Genes Exist?
What do Sickle-Cell, Cystic Fibrosis, and Tay-Sachs Diseases have in common with my familial disease?
My two siblings and I each received two pathogenic (disease causing) versions of the POLG gene, which has caused all three of us to suffer from a progressive, neuromuscular disease due to mitochondrial dysfunction. I am fortunate in that my symptoms only started in my 30s and have not prevented me from living a full life. Others with POLG gene defects (there are hundreds of varieties), such as my sister, who died early after many years of severe symptoms, and the many who suffer debilitating childhood disease onset are not so lucky.
My search to discover more about the genetic origins of my family genetic disease has led me to stumble across a much bigger question that has puzzled and challenged scientists for at least the last 70 years, and is still quite controversial to this day:
How can severely pathogenic alleles (gene variants) of many genes remain present in relatively high frequencies in the human species if Natural Selection has been acting throughout time to cause the extinction of any alleles that reduce reproductive success?
Obviously, genes mutate. However, the known mutation rate of human DNA is many orders of magnitude too low to be balanced with the known frequency of pathogenic alleles of many genes in the population (or sub groups) unless the pathogenic alleles also provide some benefit.
For example, Sickle-Cell Disease (SC), Cystic Fibrosis (CF), and Tay-Sachs Disease (TS) are each terribly debilitating genetic diseases that affect different organs, reduce life expectancy and the ability of the afflicted to reproduce. TS is always terminal in children, and SC and CF patients rarely lived until adulthood for most of human history. Each disease has plagued the human race for hundreds or (for SC) thousands of years. Pathogenic alleles for each of these diseases appear at high frequency in population subgroups such as the European whites (CF allele 4%), Ashkenazi Jews (TS allele 4%), equatorial West Africans (SC allele freq. 30%).
At first glance, these facts seem to be in conflict with the Theory of Natural Selection, which dictates that gene variants (alleles) that significantly reduce the reproductive success of individuals or the kinship group having the same allele, will be eliminated from the gene pool. So why have these diseases plagued humans for so long and the pathogenic alleles remained in the population?
The reason it seems for many pathogenic genes is a process called Heterozygote Advantage, which does not follow the simple Mendelian Genetics model with completely dominant and recessive genes controlling animal phenotypes (traits).
Many biology students have learned that all of the 22 pairs of autosomal (non-sex controlling) chromosomes in human cells provide each individual with 2 alleles, or versions for each gene. The common example given to students to describe dominant and recessive genes involves eye color. The allele for brown eyes (B) is dominant over the allele for blue eyes (b). An individual having 2 alleles for brown eyes (BB), or 1 each for blue and brown (Bb), will have brown eyes. Only an individual with two alleles for blue eyes (bb) will have blue eyes, making the b allele recessive. Cells that have two of the same allele (i.e. bb or BB) are called homozygotes. Cells with a mixture of alleles are called heterozygotes (i.e. Bb).
But in the case of Heterozygote Advantage, the recessive allele is not completely silent in heterozygotes, and it provides a benefit to the heterozygous organisms relative to individuals homozygous in the dominant allele.
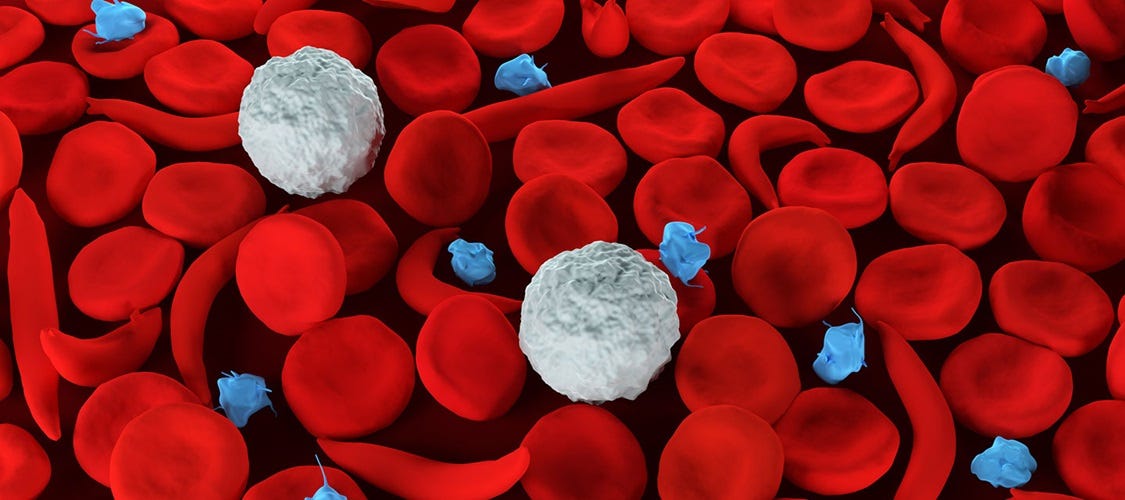
For example, those afflicted with SC disease have received from their parents two recessive alleles of the HBB gene that encode for, or instruct cells on how to produce, hemoglobin. The result for those who suffer with SC are red blood cells that are sickle shaped and are prone to clotting, causing severe pain and frequent strokes. Prior to modern medical advances those afflicted with SC disease would not typically live long enough to reproduce. However, those heterozygous individuals fortunate enough to receive only one recessive HBB allele receive partial immunity to malaria, which killed an estimated 627,000 worldwide in 2021 despite the widespread use of pesticides, breeding ground control measures, mosquito net distribution, etc.
A 1,000 children born to parents who each carry just one recessive HBB allele would include approximately 250 children (¼) who suffer from SC disease and who would likely die an early death without modern medicine. But simultaneously, approximately 500 children (½) would be born with partial immunity to malaria, which is a strong reproductive advantage.
In the brutal calculus of Natural Selection, the increased survivability and reproductivity of this heterozygous cohort “balances” the loss of the 250 SCD deaths.
Similarly, there is significant evidence of Heterozygote Advantage with the pathogenic and recessive alleles of the CFTR gene associated with Cystic Fibrosis (CF). Individuals born with two copies of recessive alleles of this Gene produce thick mucus in their lungs and airways which leads to numerous health issues and reduced lifespan and reproductivity. Heterozygotes with the most common mutated allele have reduced susceptibility to asthma, and likely other, deadlier respiratory diseases like cholera.
Tay-Sachs Disease (TS) presents a more complicated and controversial picture. TS primarily occurs in the (previously) isolated breeding population of the Ashkenazi Jews from Central Europe. TS is just one of a large number of genetic diseases that occur among the Ashkenazi at high frequency.
In 1966, N.C Myrianthopoulos presented birth and mortality data that was suggestive (but not statistically significant) of a reproductive advantage of unknown physiological basis, in those heterozygous for pathogenic TS genes. The hypothesis of heterozygote advantage was further supported by research that showed that four of the Ashkenazi diseases (TS, Gaucher disease, mucolipidosis type IV, and Niemann-Pick diseases) are results of defects in sphingolipid storage that impact neuron (i.e brain) development.
However, starting in the mid 1990s a flurry of papers rejected the need/possibility of Heterozygote Advantage with Ashkenazi diseases (see summary here). Those papers argue that the Founder Effect and Genetic Drift can explain the Ashkenazi cluster of diseases.
Not coincidentally, the famous book, The Bell Curve, by Charles Murray and Richard Herrnstein had been published in 1994; it was (and is still) highly controversial because it claimed that:
Intelligence (IQ) is partly heritable
Ashkenazi Jews have the highest average IQ of any tested ethnic group
Suddenly, a potential source of selective advantage (higher IQ) for the Ashkenazi Jews was being widely debated. In a 2006 paper, a Natural History of Ashkenazi Intelligence, the authors (Cochran et al) present considerable evidence that Heterozygote Advantage explains both the high frequency of numerous pathogenic alleles (TS, Gaucher, Niemann-Pick, and mucolipidosis type IV, BRCA1, BRCA2) and the measured high intelligence of Ashkenazi Jews relative to other Jewish populations and other ethnic groups from the same regions of Europe.
The paper is highly contested (when not ignored) in academia as are the topics of IQ, and IQ and race in particular. The evidence supporting the significant (>50%) role of heredity in determining IQ and the existence of ethnic group average IQ differences is overwhelming, but we'll leave further discussion of Nature vs. Nurture to another article. Suffice it to say, Heredity Advantage, with higher IQ being the advantage, is the most plausible explanation for the high frequency of Ashkenazi disease causing alleles. The competing theories, which postulate that a Founder Effect and Genetic Drift can explain the high frequency of these pathogenic alleles, are inadequate to explain the effect without unreasonable assumptions.
So getting back to where I started: Is there some Heterozygote Advantage for the pathogenic POLG alleles that my siblings and I all have?
The prevalence of all variants of defective POLG genes is up to 2% in some populations with European ancestry, which would argue for some kind of Heterozygote Advantage or similar genetic benefit assuming significantly reduced reproductive success for homozygotes of defective alleles.
However, the reproductivity of homozygotes is not known, and is clearly much more than 0, as many homozygotes with defective POLG alleles live into adulthood and reproduce. For example, my sibling cohort produced (thanks to the heroic efforts of my brother) slightly more than the reproductive replacement rate. All things considered, Genetic Drift following an original single mutation in Northern Europe sufficiently explains the POLG allele population distribution of today. Any advantage in my defective genes is too small to measure.
5/3/22 Update: The first version of this article neglected to mention one of the most common hereditary pathogenic gene mutations, factor V Leiden, which causes abnormal blood clotting. The high allelic frequency of the FV Leiden polymorphism in Caucasians (5–15%) prompted scientists to search for Heterozygote Advantage. It has been speculated that the enhanced blood clotting gives a survival advantage to women during childbirth, as well as to wounds, as might be incurred in conflicts. There is no evidence of this however. There is solid evidence that heterozygotes have significantly greater survival rates for sepsis and exposure to the plague. The question remains though as to why and how factor V Leiden developed only in Europeans (apparently over 20,000 years ago) and well before the plague evolved into it’s modern form.